In the 2018 Medscape Survey on Physician Burnout and Depression, over 15,500 physicians were surveyed. The Medscape survey was aimed at answering some vital questions, such as “What causes physician burnout?” and “What are some ways to fix physician burnout?” The results were interesting, and I think worth discussing.
Today, we will highlight some of the results and how these facts might impact our decisions around burnout at work.
The Basics
Of the more than 15,500 surveyed, 61% were men and 39% were women. The survey was collected over a four month period (July to October) and it was sent to both Medscape members and non-member physicians practicing medicine only in the United States.
Interestingly, the percentage of physicians that were burned out was 42% regardless of whether they worked as an employed physician or were self-employed.
What is the prevalence of burnout in each specialty? Here are the numbers:
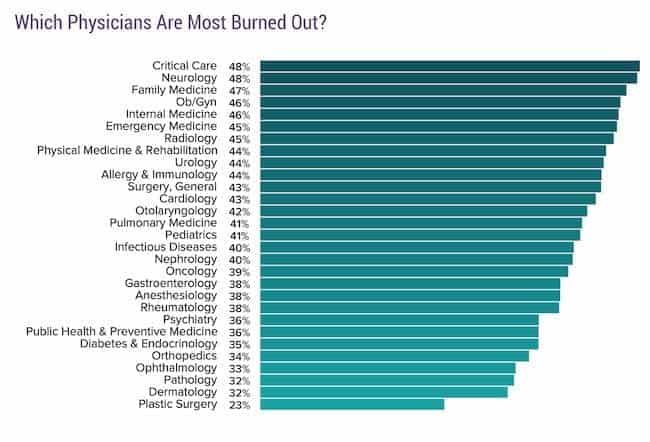 In all, over 26 specialties had a burnout rate of 33% or higher. In essence, one in three colleagues were burned out. Some studies have suggested much higher rates. This went as high as almost one in every two for critical care and neurology.
In all, over 26 specialties had a burnout rate of 33% or higher. In essence, one in three colleagues were burned out. Some studies have suggested much higher rates. This went as high as almost one in every two for critical care and neurology.
One finding that surprised me from the prevalence results was how high the numbers were for specialties that are often considered “less stressful” (i.e. family medicine, PM&R, etc). As we look at the causes of burnout below, it might not be so surprising anymore.
Big Picture Causes of Depression
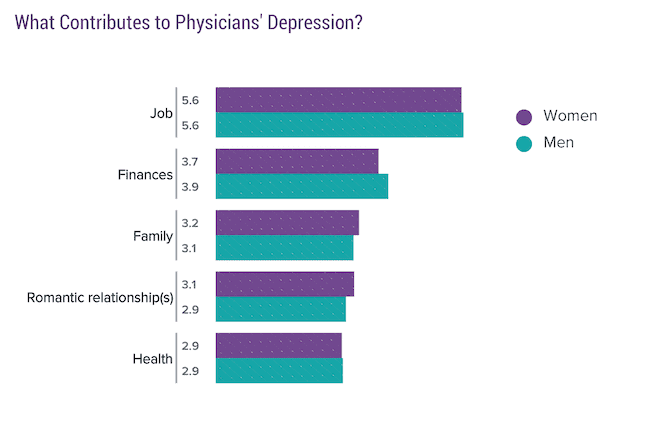
The respondents were asked to determine various big picture etiologies of their depression from several different categories. These results are below. It turns out that the number one cause was their job.
Interestingly, the number 2 cause was finances.
Given that the purpose of this website is to help combat burnout through financial independence, this didn’t surprise me… but it was nice to see the thought validated in a survey.
Causes of Burnout and Ways to Reduce It
Now, this was the most interesting information from the entire study. Physicians were asked to determine the causes of burnout. Then, they were encouraged to label some ways that burnout/depression might be reduced.
We already determined from the above information that the second leading cause of depression seems to be financial. That said, when asked about specifics at work that caused or led to burnout this is what the respondents said:
You would think from the top two causes (too much bureaucratic work and spending too much time in the workplace) that the obvious ways to help minimize these problems would be for physicians to ask for secretarial help, scribes to help them chart, and to pursue partial FIRE (to allow more time away from work).
But, that’s not what the people responding to this survey said.
In typical physician fashion, they demanded more pay to compensate for their stress. Apparently, doctors don’t make enough money. So that I avoid putting words in their mouth I’ll show you what they said and then discuss my thoughts below:
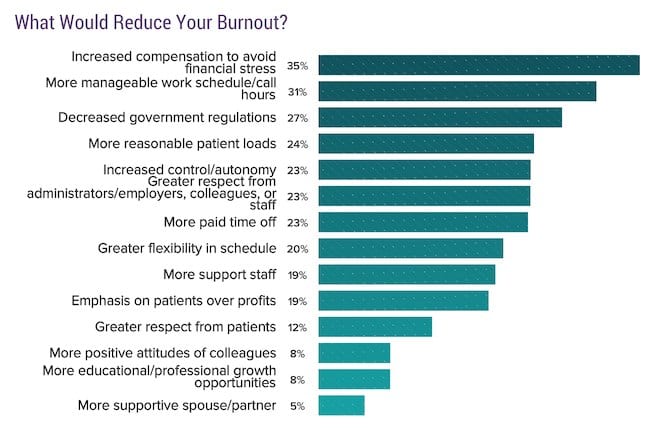 What do you think about the responses? Over a third of the doctors in this study thought that being paid more would lead to less burnout. This is despite the causes that listed above where money isn’t mentioned until the fifth cause for burnout.
What do you think about the responses? Over a third of the doctors in this study thought that being paid more would lead to less burnout. This is despite the causes that listed above where money isn’t mentioned until the fifth cause for burnout.
My Thoughts
I think this survey can be broken up into two difference sources of frustration: the big picture (work-life balance) and the little picture (causes of burnout at work).
The Big Picture
In the big picture, finances seem to play a large role. We see this twice. First in the causes of depression where finances are listed as the number 2 cause only behind the workplace. This goes to show that finances can be directly linked to depression and burnout.
The solution to this problem isn’t to pay physicians more, but to give them a higher financial literacy coming out of training so that they know what to do with the money that they receive. Financial Independence can help solve a lot of these problems, if only physicians were taught about this stuff.
What kind of stuff? Well, like the fact that physicians have a spending problem. When burnout comes raging into the physician life, a lot of people think the answer is to spend money to find the happiness that is missing. This is like adding water to a grease fire.
Yet, when physicians were asked what could solve the burnout problem, the number one solution provided was to increase their pay. My gut feeling is that most doctors would not feel this way if they knew how to handle their money.
To be clear, I am not arguing that paying physicians more is a bad idea – I just don’t think it would solve the problem of burnout.
The Little Picture
I could have been a doc surveyed with the question “What contributes to physician burnout?” I would have given similar answers.
The fact is that non-physician tasks have continued to creep into the workplace for doctors. We have more charting, more electronic billing, more administrative creep, and less time taking care of patients. Many doctors also do not have work-life balance as they spend too much time at work. Hospital administrators who refuse to put employees first don’t help either.
These answers make sense. They are definite contributors to burnout. As physicians, our job is to take really good care of people, to bill them for their care (to keep the doors open), and – if you are in academia – to teach and to perform research.
Anything that is not inherently involved in those tasks should be supported by work staff who can help contribute to a decreased physician work-load. Personally, I’ve felt the burn lately and it mostly results from an ever growing “to-do” list that I can’t seem to get done.
Ironically, though, these same doctors filling out this survey said that getting paid more would remedy these problems. How does getting paid decrease meaningless tasks, lessen work demands, or give you more support from administration?
This is a prime example of people who don’t understand The Tale of Two Doctors. They’ve likely financed a life that they cannot afford in an attempt to make them happy. In other words, it seems like a lot of Dr. Jones’ filled out this survey.
Take Home
Looking into the prevalence and causes of burnout among physicians is a really important task. While it seems that we have done a good job of determining causes, we did not do the best job highlighting what the best fixes might be for the problems we face.
In the end, I maintain that teaching financial literacy to medical students, residents, and early career attending physicians will help prevent a lot of the financial causes of burnout. Also, It will allow these physicians to have a better work-life balance as they approach financial independence and have more options.
What did you think about the survey results? What was your take away? Leave some comments below.


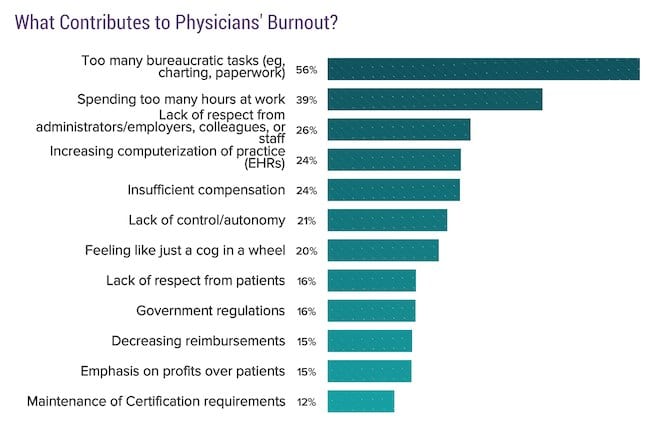



Wow interesting stuff. It struck me that basically bureaucracy is the leading cause of stress. In my job as a manager of a large office I would say it’s the same. With automation and artificial intelligence being all the rage these days in the technology world, you would think we would have ways to solve many of these bureaucratic tasks
You’d think. In the world of medicine that would involve putting the physicians first and providing said services. Unfortunately, scribes and electronic solutions cost money, which cuts into the bottom line.
I for one can tell you that increased pay does not indeed reduce burnout so I do find that a bit odd that physicians think that would be a cure-all.
I am highly compensated even with regards to my specialty (sort of blow the average salary reported by MAGA out of the water) but knowing I am getting paid a lot still does not make the meaningless tasks that more tolerable.
I agree with your point that if physicians had any sort of financial acumen that it would be the best way to combat burnout as you can slow down your practice/take extra time off or remove parts of your practice you don’t like doing if possible (such as Hatton removing OB from her practice or me taking 1 day off a week).
Glad we are on the same page. More money will not solve the problem in medicine. Higher financial literacy just might… as options and time are really what most doctors are searching for. It will take a critical mass to get there, though.
This is important information that we should all be talking about. I’m adding it to my financial independence talk! Your take on how people view the fix is inciteful. We always assume we can buy our way to happiness but once basic needs are met that isn’t true. We need to do the hard work of fixing the problems with medicine
Glad to help provide some perspective! This information is important to get out there.
Interesting results. I agree that more compensation is not the solution to burnout. The other stuff would help more- manageable work hours, more time off, manageable pt load, more autonomy. Also eliminating the BS busywork is half the battle.
Completely agree. Decreasing non-physician tasks, scut work, and just all around meaningless tasks would be a start. It always amazes me how the little things (paperwork, submitting monthly work sheets, forms, licenses, etc) burns me out so much faster than the big things (patient care, education, research). If I could just focus on the big things, I bet I’d be super happy.
I totally agree. A better fix would be to improve financial literacy among physicians. That way, when we actually do get paid more… we know what to do with our money and it won’t cause us as much stress.
To be honest, I’m surprised that general surgery is relatively low on the list. And where’s neurosurgery? I did not expect PM&R to have a high burnout rate… I thought it stands for “plenty of money and relaxation” 😉
Completely agree. This year’s results were shocking in terms of the specialties that were represented and in what order. Found that fascinating.
And the funny thing about money is that no amount of increased money fixes poor financial literacy. Without the latter, you could have Scrooge McDuck piles of money and there would still be massive issues.
When I was really in the thick of my burnout struggle, I remember grasping at the increase in salary as a way to help me out of it though it ultimately wasn’t a true solution.
I think it’s a real, tangible way for us to find a “fix” or at least to justify why you feel like you’re at work all the time. Even when I wasn’t at work, I was always thinking about it as the job became all-consuming.
The other component to it is if you can negotiate a salary increase, you can then justify cutting back a little to get to your same previous salary. It’s twisted in how I had to game the system, but this is what I did.
Ultimately it wasn’t about the money – it was being able to cut back and still financially hit my goals aka get ahead on my student loan debt
It’s always about having options and being able to design the life we want to live. The ultimate commodity is time. Money simply affords us these options. When we aim for money instead of the real goal, we miss our target and settle for worsened burnout.
The problem is that the real “fixes” are not in our control. Hence, why we don’t really consider them as an option for fixing burnout.
A third think that more compensation would reduce their financial stress!??! Absurd! Can you believe these people are doctors? They are smart, right? They form opinions based on evidence, right? Wow!
No, when you are in the top 5% for household income in the U.S. earning an even higher salary will NOT reduce your financial stress people! Don’t you want to shake them? Learn to better manage the overabundance of money you have folks. You won the game of offense. Focus on defense now. Saving, investing, lowering expenses, and avoiding catastrophic losses. A bonus or side gig will not help.
Agreed, wealthy doc. But it’s the upside down world we live in… And these people are smart, they just haven’t ever been taught any better.
It’s like complaining that someone doesn’t know what Occam’s Razor is or what an ontological argument is… Stuff I wouldn’t expect most non philosophy majors to have studied.
It’s a big reason we need to open their eyes.
Many of us in the corporate healthcare setting are burned out by the patient satisfaction push that administrators impose on us, along with a gazillion clicks on a poorly constructed EHR.
I do think that higher pay does blunt the insult slightly, but only as a means to get through to FIRE sooner. Getting an extra $150 if I do an overnight shift doesn’t cut it, however!
Getting more money to accomplish FIRE faster only counts if you know what to do with the money when you get it.
Most of these doctors filling out that survey would simply spend it because they don’t know how to properly build wealth.
I do agree that if you know what you are doing (and have the discipline to do it) that getting paid more might provide options sooner.
The “solution” voted for by many survey participants is THE problem: being paid more does not equal happiness. It is assumed in our culture that this will help, but it won’t. A change in culture and values is the solution, and more financial literacy as you’ve proposed is a big part of that, along with wider acceptance of part time or alternative work hour arrangements.
Funny, as an anesthesiologist I always feel that the development of EMR has helped our field have less burnout (I hate charting vitals while taking care of patients in the OR!)
Thanks for your analysis of this data.
Completely agree on everything you are saying. I actually have a couple posts coming up on this subject (contentment, money not equating to happiness, etc).
P.s. charting vitals manually is painful so long as people can pay attention when they aren’t having to chart them!
Like Dave Ramsey would say, you cannot out earn your stupidity. The more doctors earn, the more they feel they need to earn. It never solves the problem. Interesting study. I agree with your conclusions thephysicianphilosopher
Haha… That’s actually really true.
You know what we say in anesthesia? “You can’t fix stupid, but you sure can sedate it.” 🙂
Many of the causes in the survey can be aggregated into loss of autonomy. There are other surveys that stratify by age, with burnout peaking in late career, suggesting that it might be related to loss of what physicians once had, whether indepence, income, peer collegiality more noticeable to those who once had them than to those who never had them.
Increasing income might help, but as the spending model suggests, attempts to buy happiness with consumer spending of augmented income creates its own problems.
Being recently retired, with a tinge of burnout, I would also question whether making physicians technocrats with no duties other than seeing patients corrects the problem. The happiest colleagues seem to be the folks who have committee work, not just showing up, but designing improvements or reviewing safety data and the like. Same with research, where the only senior physicians at my recent national meetings seem to be the professors with active labs. They may be the only people who can afford to go.
Since we cannot make the EHR disappear and the economies imposed by payers at least have some rationale that physicians cannot abandon, the best prospect would be to better cope with that reality. I think a better solution than more pay would be well defined protected time to pursue non-clinical medically contributory pursuits such as quality improvement or teaching. The time needs to be well defined by the employer and to keep it from being frittered or absorbed by momentary urgencies, the physician also needs an obligation to have a written plan of how that time is to be used and what reasonable accomplishments would be. The real solution to burnout may in the end be accomplishment that is really worth the effort of the person doing the work and appreciated by the recipient.
Completely agree that loss of autonomy and lack of support to pursue satisfying/fulfilling projects are the main contributors to burn out.
Any change that would increase those endevaors (autonomy, projects, protected time, etc) is sure to better the burnout problem.
Thanks for your thoughtful comment!